- Home
- About the Journal
- Peer Review
- Editorial Board
- For Authors
- Reviewer Recognition
- Archive
- Contact
- Impressum
- EWG e.V.
DOI 10.35630/2022/12/psy.ro.35
Increased survival of oncology patients brings to attention new aspects of adverse effects due to antineoplastic treatment. Psychiatric disorders, cardiovascular disorders as well as the progressive incidence of multiple primary neoplasia are some of the most common side effects. Aim: Care of the oncology patient undergoes an important period of change, from the management of tumor disease to the multidisciplinary approach, centered on improving the quality of life. Method: We present the case of a 75-year-old patient, whose personal pathological history reveals the presence of a diagnosis of left testicular seminoma, in 1978, for which he received radiochemical therapy. An oncological patient under long-term medical supervision for several decades is diagnosed in November 2017 with urothelial carcinoma, infiltrative, invasive in his own muscle patch, pT2NxMx. Approximately 40 years later, the second neoplastic site, the malignant bladder tumor, appears. Facing this diagnosis, the patient becomes anxious, anticipates catastrophic consequences, isolates himself. The family and friends support is essential in these moments, the patient tries cognitive-behavioral psychotherapy, as well as various relaxation techniques, which have positive results for the patient attitude towards the disease. He admits, to complete staging, to follow the recommendations of the oncologist, perform proton emission tomography, which detects the presence of two lesions on the right lung. In January 2018, the surgical intervention is done by straight thoracotomy, atypical upper lobe resection and inferior lobectomy is performed. The histopathological and immunohistochemical results describe the presence of the third primary adenocarcinoma neoplasia. The initial emotional reaction is one of anger, denial, followed by demoralization, easy crying, sadness. The patient is examined by the psychiatrist, thus receiving the diagnosis of a severe depressive episode without psychotic symptoms. He follows an anxiolytic, antidepressant, sedative treatment but continues also the cognitive-behavioral therapy. The patient shows good compliance with psychopharmacological treatment and accepts adjuvant chemotherapy courses, which are well tolerated. Throughout the antineoplastic therapy, there was a close collaboration between the psychiatrist and the oncologist, to avoid drug interactions that could have led to interruption of the treatment. Under the oncology supervision, the patient receives another bad news, in September 2018, the fourth neoplastic localization, the prostatic adenocarcinoma pT2bN0M0, is discovered. In this case, in the presence of the combination of synchronous and methacrone tumors, the patient's psyche is deeply affected, continuing the psychopharmacological treatment. Conclusions: Psychiatric disorders are common among oncological patients, and they may suffer serious impairments in quality of life and treatment compliance, psycho-oncological collaboration being indispensable for the success of antineoplastic treatment.
Keywords: Multiple primary neoplasia, depression, oncology patient, treatment.
Within the framework of recent statistics, therapeutic advances have improved the survival of oncology patients (Koch et al., 2013). The World Health Organization estimates an increase in the incidence of neoplastic diseases in the coming years, the number of deaths due to oncological diseases will reach Romania in 2040 to 60,000, so cancer remains one of the diseases with a significant psychosocial impact (WHO, 2020).
Care of the oncology patient goes through an important period of change, from the management of tumor disease to the approach centered on improving its quality of life (Ciobotea et al., 2016; Pop et al., 2016).
Psycho-oncology, as part of interdisciplinary medicine, involves communication and cooperation between specialists in different medical and non-medical fields (Caras & Sandu, 2013; Sandu, 2013), proposing to promote patient accountability and increase its participation in decision-making,of the compliance with the therapeutic program and implicitly increasing its satisfaction with regard to treatment (Pop et al., 2016).
The prevalence of psychological-psychiatric disorders in cancer patients is estimated in some 47% of studies, of which anxiety and depression 68%, 13% major depression, 8% delirium (Bogdan & Bogdan, 2015; Newport & Nemeroff, 1998). Identifying depression in oncology patients is difficult. Depression can easily be overlooked because cancer symptoms and its treatment resemble the neurovegetative symptoms of depression, such as fatigue, loss of appetite and sleep disturbance (Greer & Watson, 1987).
A number of researchers have studied the emotional reactions of people with cancer. Greer and Watson (Greer & Watson, 1987) observed and described five characteristic patient responses to cancer diagnosis. Survivors of a cancer can develop certain psychiatric disorders during their lifetime or at the time of recurrence diagnosis, requiring psychotherapy and specialized treatment (Ionescu, 1990; Simard et al., 2013). The emotional response of the person with cancer is determined by three factors: the point of view of the diagnosis, the perception of disease control, and the vision of the prognosis (Clarke, 2010; Lupu et al., 2016).
We present the case of a 75-year-old urban patient with a performance index (IP) = 1, insignificant heredocolateral (AHC) antecedents, of particular importance are the personal pathological antecedents that draw attention to the existence in 1978 of a diagnosis of the left testicular seminoma , for which the patient underwent polychimioterapic therapy and total dose (DT) = 40 Gray radiotherapy. After the treatment, the patient was declared cured but remained under oncology for 5 years, during no recurrence was detected. Concerned about his state of health, the patient continues oncology monitoring for a long time, being considered free of illness for several decades.
In the 2017 oncology re-evaluation, the CT scan performed for the thorax, abdomen and contrast pelvis (SC) reveals the presence of a 5mm long, right-lined basal lymph node. Parietal bladder changes with possible tumor substrate (Fig. 1a) Prostate with dimensions 30/36 mm, median lobar hypertrophy and bladder footprint (Fig.1.b) No free fluid in the peritoneal cavity. Prostate specific antigen (PSA) value = 4.38ng / ml.
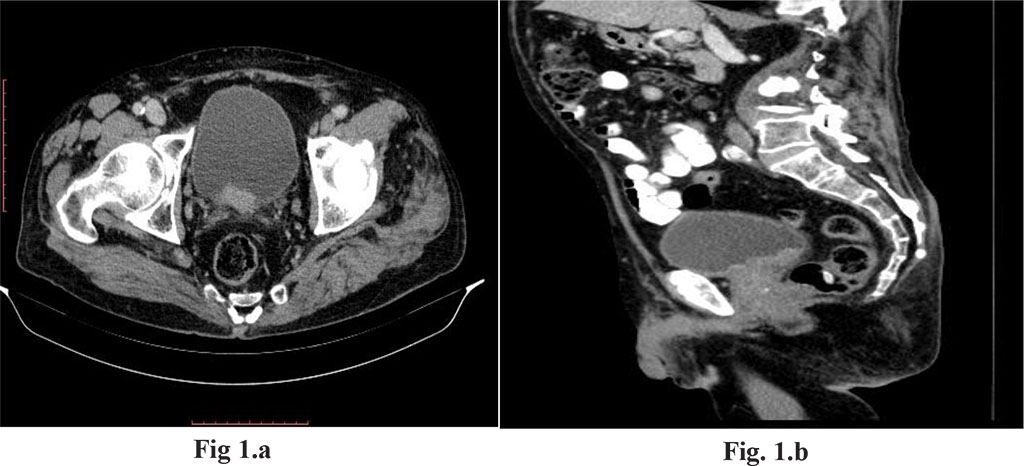
Fig 1.a CT
image axial plan, Parietal bladder changes
Fig.
1.b CT image sagital plan,
Prostatic hypertrophy
Source: Authors' own conception
The patient is referred to the urology service where he receives a recommendation to perform a prostatic biopsy and a cystoscopy. In November 2017 , cystoscopy is performed with transurethral resection of a ¾ cm formation, centered on the right ureteral opening, with favorable later evolution. The result of the histopathological (HP) examination, high-invasive urothelial carcinoma, invasive in the bladder-like muscle. There is no lymphovascular or perineural invasion. Staging of tumor metastasis (TNM) -pT2NxMx.
Faceing a new oncology diagnosis, the patient anticipates catastrophic consequences, becomes anxious, isolates himself, refuses any medical help. Family and friends are actively involved in improving mental health, using individual and group cognitive behavioral therapies in order to understand the situation they are crossing, to regain communication with others, but also with the hope that they will managed to defeat cancer this time. The combination of psychotherapy and relaxation techniques to which the patient is appealing changes his attitude towards the disease and accepts that, in order to complete the staging, he should follow the recommendations of the oncologist. He performs a CT scan (PET / CT) Whole Body, that detects the presence of an active metabolic knot (SUV = 5.03), located in the posterior segment of the upper right lobe, with dimensions of 13/12 mm. Metabolically active pseudo nodal lesion (SUV = 2.42), located in the postero-basal segment of the right lower lobe, with dimensions of 36/21 mm. Pulmonary CT and PET lesions comparable to an ’in situ’ bronchial-alveolar invasive mucosal carcinoma.
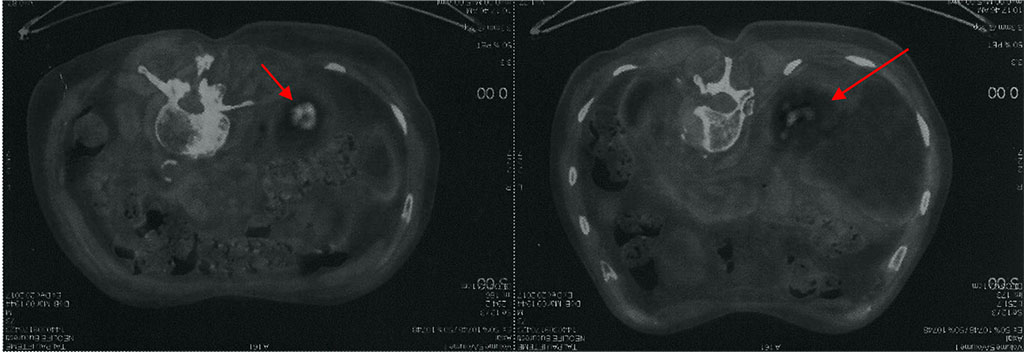
Fig.
2. PET / CT image active metabolic node active upper right lobe (left)
and metabolically active pseudo-nodular lesion inferior lobe right
(right)
Source:
Authors' own conception
The consultation practised in the thoracic surgery service recommends the surgical resection of the two metabolically active formations, following spirometry and fibrobronchoscopy. In January 2018, a right thoracotomy was surgically performed, and FOWLER segment was invisible, with an invasion in the dorsal segment of the upper right lobe, a node approximately 2 cm excised by atypical lung resection. In the right inferior lobe, there is an imprecisely defined tumor of approximately 3.5-4 cm, for which inferior lobectomy is performed. The histopathological and immunohistochemical result (IHC) describes the presence of the third primary neoplasia primitive pulmonary adenocarcinoma. Staging pT4N0. The genetic status that identifies the epidermal growth factor receptor (EGFR) mutant exon 20 is evaluated (Shepherd et al., 2005). Emotional response to the diagnosis is firstly emotional immobility, followed by denial, seeking answers. Later, anger, demoralization, easy crying, sad, feel that all physical suffering and endeavor so far have been in vain, its vision of prognosis is bleak. He goes to the psychiatrist, receives the diagnosis of a severe depressive episode without psychotic symptoms. Following anxiolytic, antidepressant, sedative treatment, the psychotherapy sessions continue to be combined with relaxation techniques. The entire therapeutic arsenal helps the patient change his perception of prognosis and accepts chemotherapy, performs adjuvant chemotherapy, 4 series with good adherence to treatment. It respects the recommendations of the oncologist, examines the MRI (RM) ,that describes the presence of diffuse cortical atrophy and fronto-parietal subcortical lesions with vasculo-degenerative aspect.
The oncological re-evaluation in August 2018, biological constants are within normal limits with PSA exception = 6.54 ng / ml, thoracic CT examination, abdomen, native pelvis and contrast substance describe the pleuro-pulmonary aspect of the stationary aspect. Liver with normal size, homogeneous structure. Modified degenerative-arthrosic changes in the thoracic and lumbar spine. No bone damage suggestive of secondary determinations. RM pelvis 3 Tesla concludes a minimal deformation of the bladder in the lateral and posterior walls in the ½ right, with its thinning and parietal thickening in rest, without tumor masses. Prostate hypertrophy of adenomatous appearance of the central prostate and with the presence of an area raising the suspicion of an adenocarcinoma in the peripheral prosthesis of the right lobe.
The patient is referred to the urology service, where he will perform ecogydate multiple prostate biopsy. The result of HP and IHC prostatic adenocarcinoma acinar, Gleason score 6 (3 + 3) highlights the presence of the fourth primary malignancy, malignant tumor (TM) of the prostate. Staging pT2bN0M0. The therapeutic decision is difficult for this patient, radical cystectomy with neoplastic might be a alternative of treatment with a curative visa, involving two of the four cancers (Autier et al., 2007; Klotz, 2004; Thompson et al., 2006). Taking into account the profoundly affected psychic, the age, the low degree of aggressiveness of the prostate tumor, but also the personal pathological antecedents, the active surveillance with 3-month PSA dosing is decided and pelvic MR. Under these circumstances, in the presence of synchronous and metacrone tumors, the patient remains under psychopharmacological treatment (Paduraru et al.,, 2019; Rebegea et al., 2019).
Oncological surveillance is an extremely important stage in the management of tumor disease, with improved antineoplastic therapies and increasing survival of these patients, there are new problems emerging from the treatment of this disease. Tumor recurrences or the appearance of another cancer during the life of the oncological patient require long - term surveillance. Multiple primary neoplasms are a reality in oncology.
The multidisciplinary approach of the oncology patient is paramount, interdisciplinary collaboration being indispensable for the success of antineopathic treatment.
Before the cancer diagnosis, the patient reacts by trying to adapt to the idea of oncological disease, but also to accept the treatment that is sometimes difficult to endure. [Emotional symptoms can be missed or even viewed with distrust, minimized, being seen by family and friends as side effects of treatment or as a consequence of disease progression.
Patients with such neuropsychiatric disorders require entourage support as well as specialized help. Psychiatric disorders are common in these patients and without psychiatric support they may suffer serious issues regarding the quality of life and compliance to treatment.