- Home
- About the Journal
- Peer Review
- Editorial Board
- For Authors
- Reviewer Recognition
- Archive
- Contact
- Impressum
- EWG e.V.
Cite as: Archiv EuroMedica. 2025. 15; 4. DOI 10.35630/2025/15/4.007
Oral squamous cell carcinoma (OSCC) remains a significant global health concern, with high morbidity and mortality largely attributable to delayed diagnosis. Despite the accessibility of the oral cavity for clinical inspection and the presence of well-established risk factors, a considerable proportion of cases are still identified at advanced stages. This report presents a case of rapid tumor progression in a patient without classical risk factors.
A 44-year-old male with no history of tobacco or alcohol use, systemic illness, or familial cancer, presented with a lateral tongue ulcer attributed to trauma. Clinical examination revealed a 10 x 14 mm lesion. Biopsy was initially postponed due to lack of consent, and conservative treatment was administered. Temporary improvement was observed. However, within 20 days, the lesion markedly enlarged. Urgent biopsy confirmed moderately differentiated OSCC. The tumor was staged as T4N0M0 according to AJCC 8th edition. The patient underwent hemiglossectomy, bilateral neck dissection, and adjuvant radiochemotherapy. Although remission was achieved, the patient died of pneumonia one week after completing treatment.
This case highlights the potential for rapid OSCC progression in low-risk individuals and emphasizes the need for immediate diagnostic action in the presence of suspicious oral lesions. Conventional oral examination must be followed by biopsy when malignancy is suspected. Early multidisciplinary collaboration and clear patient communication are essential to avoid preventable delays and improve clinical outcomes.
Keywords: oral squamous cell carcinoma; diagnostic delay; early detection; tongue cancer; case report; interdisciplinary care
Squamous cell carcinoma (SCC) is the most prevalent malignancy of the oral cavity, accounting for up to 90% of all head and neck cancers [1]. According to the World Health Organization (WHO), oral cancer includes malignancies of the lips and other parts of the mouth, and in some classifications, it also encompasses the oropharynx [2,3]. As reported by the Global Cancer Observatory (GCO), in 2022, oral cancer ranked 16th among all malignancies worldwide, with an estimated 389,846 new cases annually [4]. Projections from the International Agency for Research on Cancer (IARC) indicate a potential increase to over 600,000 new cases per year by 2045 [5].
The disease predominantly affects men over 50 years of age, with the ventrolateral tongue and the floor of the mouth identified as the most common sites [6]. Major risk factors include tobacco use, alcohol consumption, and their combined effect, which can increase the risk of developing oral cancer up to 38-fold compared to non-users [7,8]. Additional contributors include chronic mucosal trauma, human papillomavirus (HPV) infection, betel nut chewing, ultraviolet radiation exposure, and a diet deficient in antioxidants [1,8].
Oral squamous cell carcinoma (OSCC) rarely arises de novo. In most cases, it develops from oral potentially malignant disorders (OPMDs), which are defined as mucosal lesions with an increased risk of malignant transformation. According to the WHO classification, leukoplakia is the most common OPMD, with a variable risk depending on its histopathological features and anatomical site. Erythroplakia, although less prevalent, exhibits the highest rate of malignant transformation, with carcinoma already present in up to 51% of cases at the time of biopsy [1,9]. Other OPMDs include submucous fibrosis, actinic cheilitis, dyskeratosis congenita, lichen planus, lupus erythematosus, graft-versus-host disease (GVHD), and palatal changes associated with reverse smoking [9].
Despite the accessibility of the oral cavity and the availability of routine dental examinations, the five-year survival rate for OSCC remains relatively low, ranging from 55% to 68%, depending on the country and population studied [10,11]. This unfavorable prognosis is primarily due to the high proportion of late-stage diagnoses. In light of these epidemiological trends, the IARC established a working group in 2021 to assess evidence-based strategies for the primary and secondary prevention of oral cancer. Their findings were compiled into the IARC manual Oral Cancer Prevention, a comprehensive resource designed to guide healthcare professionals in identifying risk factors and implementing effective prevention programs [1].
This report presents a case of rapidly progressing OSCC in a systemically healthy, low-risk patient, underscoring the importance of early detection, patient awareness, and interdisciplinary collaboration in improving clinical outcomes.
On January 3rd, 2023, a 44-year-old male patient presented to the clinic reporting a lesion on the tongue. The lesion had occurred approximately three months earlier due to trauma, specifically “biting the tongue”, and had caused persistent discomfort since then, with a reported pain level of 2 on the Visual Analog Scale (VAS = 2). The patient's general condition was assessed as good. He reported no known comorbidities, no significant medical history, and no habits of smoking or heavy alcohol consumption. There was also no relevant oncological family history. During the extraoral examination, no abnormalities were detected, including no enlarged regional lymph nodes in the submandibular, submental, facial, or cervical regions. However, the intraoral examination revealed insufficient oral hygiene, moderate dental calculus, and sharp cusps of the lower molars, which may have contributed to the trauma. Salivary flow and the overall status of the oral mucosa were normal.
As part of cancer prevention, a conventional oral examination (COE) was performed under appropriate lighting. On the left lateral surface of the tongue, corresponding to lower left molars, an exophytic lesion measuring 10 x 14 mm was identified (Fig. 1A). The lesion presented as a vivid red ulcer with irregular, well-defined edges and a firm base covered with fibrin, located on inflamed tissue. It was markedly tender on palpation, though tongue mobility remained preserved. Chronic irritation by molar cusps was observed.
The biopsy had to be delayed due to the lack of informed consent, prompting a 7-day follow-up period. Initial interventions included the correction of sharp tooth edges, local anti-inflammatory and antiseptic treatment, and professional mechanical plaque removal, followed by oral hygiene instructions. Blood tests, including a complete blood count with differential and inflammatory markers (ESR, CRP), were ordered. A swab from the dorsal surface of the tongue was also taken for mycological examination.
By January 10th, follow-up showed significant local improvement (Fig. 1B). The pain had ceased (VAS = 0), and the lesion had decreased in size to 7 x 9 mm. Epithelialization was observed at the ulcer base, and the lesion’s borders had reduced. Both the inflammatory background and tenderness had subsided. Laboratory blood tests revealed no abnormalities, and Candida spp. were not cultured. Based on these findings, it was decided to continue the anti-inflammatory treatment, and another follow-up appointment was scheduled. The patient was instructed to monitor the lesion and seek immediate medical attention in the case of symptom recurrence or lesion progression.
On January 30th, twenty days later, the patient returned prior to the scheduled follow-up due to pain recurrence. He reported persistent pain for approximately one week (VAS = 4) and stated that he had consulted another physician in the interim, though no interventions had been undertaken. Extraoral examination revealed enlargement of the submandibular lymph nodes (group 1B). Intraoral examination showed significant progression of the lesion, which had increased in size to 12 x 16 mm (Fig. 1C). The ulcer, situated on inflamed tissue, had prominent, indurated, raised edges and palpable infiltration at the base. After a brief discussion and obtaining informed consent, an urgent oral biopsy was performed.
By February 9th, histopathological analysis confirmed a moderately differentiated (G2), partially keratinized squamous cell carcinoma. Clinically, there was marked progression - the crateriform ulcer with irregular, thickened edges had nearly doubled in size to 21 x 29 mm (Fig. 1D). The patient was promptly referred for further oncological evaluation and treatment.
On February 28th, the patient was admitted to the oncology department. The tumor was staged as T4N0M0 (AJCC 8th edition) carcinoma of the tongue body. Combined therapy was initiated, including resection of the left half of the tongue along with the floor of the mouth up to the tongue root, bilateral neck dissection (levels I-IV), and adjuvant concomitant radiochemotherapy. The final ENT evaluation confirmed complete remission. However, one week after the completion of treatment, the patient died from pneumonia.
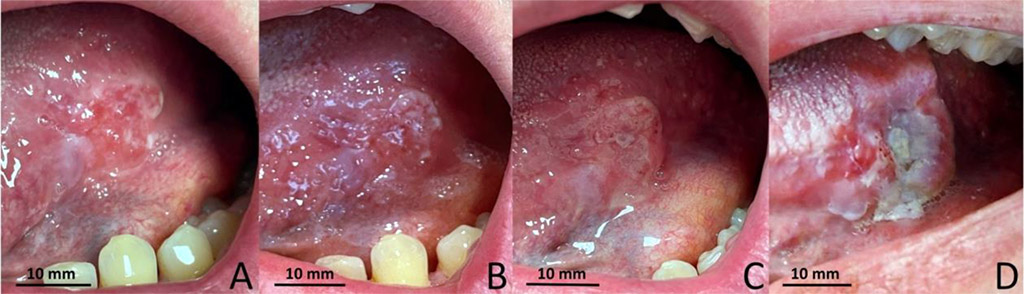
Fig. 1 Progression of the lesion: A - 03.01.2023; B - 10.01.2023; C - 30.01.2023; D - 09.02.2023.
According to the IARC manual “Oral Cancer Prevention,” secondary individual prevention, which involves early detection and treatment of malignancies and OPMDs, should begin with risk assessment and appropriate patient stratification. This enables clinicians to tailor preventive strategies to each patient's clinical situation. High-risk individuals require enhanced monitoring and regular screenings [1]. However, diagnostic challenges and preventive shortcomings can arise when patients do not exhibit classical risk factors, potentially leading to delayed diagnosis. This was evident in the presented case of a 44-year-old male who did not smoke or consume alcohol, was systemically healthy, and had no family history of cancer. The only identified risk factor was chronic mechanical trauma, which may have acted as both a trigger and a promoter of malignant transformation. Furthermore, the patient delayed seeking medical care for three months prior to his first visit, limiting the window for early intervention. This case underscores the critical importance of both clinician and patient oncological vigilance to ensure timely diagnosis and treatment.
Studies from Eastern Europe, China, the United States, and Australia indicate that public awareness regarding oral cancer, its risk factors, and early symptoms remains insufficient. While tobacco is widely recognized as a carcinogen, alcohol consumption, advanced age, and persistent mechanical trauma are rarely acknowledged by the general public as contributing factors [12-16]. In this case, the patient sought medical attention three months after experiencing tongue trauma, despite persistent pain and ongoing irritation from molar cusps. Greater cancer awareness may have led to earlier consultation, potentially shortening the diagnostic timeline and improving prognosis. Research also shows lower oncological awareness in older populations. Although this suggests potential improvement in future generations, middle-aged individuals remain at elevated risk, underscoring the urgency of targeted education and increased preventive efforts among this demographic [12-13].
Population-level strategies, including screening programs and public health campaigns, are essential to improving the overall epidemiological outlook [17]. At the same time, dentists, as frontline healthcare providers, play a crucial role in individual cancer prevention. This case reflects broader trends identified in current research, including gaps in both public and, at times, professional knowledge. It highlights the need for systemic educational reinforcement aimed at increasing awareness of risk factors, early signs of oral cancer, and the importance of prompt intervention [12-16,18]. Furthermore, this case reflects a shifting oncological profile, with oral cancers increasingly diagnosed in younger, systemically healthy individuals lacking classical risk factors. Continuous surveillance of emerging evidence and the adaptation of preventive strategies are, therefore, imperative [1].
During the initial visit, the patient underwent a conventional oral examination (COE), which remains the gold standard for oral cancer screening. This technique involves a thorough evaluation of all oral anatomical sites under proper lighting. Despite its simplicity, COE has demonstrated good diagnostic sensitivity and specificity [19-21]. A 2022 meta-analysis by Essat et al. reported a sensitivity of 71% and specificity of 85% for COE in detecting dysplastic lesions, compared to histopathological evaluation [19]. Although adjunctive tools such as toluidine blue staining, brush biopsy cytology, and autofluorescence imaging exist, current evidence does not support their superiority over COE [22]. Nevertheless, in cases such as the one described, these methods may serve as communication tools that help visualize the lesion and motivate the patient to comply more quickly with biopsy recommendations, thereby expediting diagnosis and treatment.
Diagnostic delay, defined as the time from symptom onset to the initiation of effective therapy, is a critical determinant of oncologic outcomes. The causes of delay often involve both patient-related and healthcare system-related factors [23,24]. A Dutch study by van der Waal et al. found the average diagnostic delay to be 206 days, with 104 days attributed to the patient and 102 to the healthcare system. The longest delay (36 days) occurred between the initial consultation and the performance of a biopsy [24]. In the present case, the total delay yields approximately 180 days, equally divided between patient- and system-related factors. From the first visit to biopsy, 27 days elapsed, an improvement relative to the literature, but still suboptimal given the aggressiveness of the tumor. This highlights the need for ongoing optimization of diagnostic workflows.
A 2021 systematic review identified limited oncologic awareness as the leading cause of diagnostic delay among patients. Underestimation of symptoms -especially in the absence of pain or functional impairment, which is typical in early stages of oral cancer, and lack of self-monitoring, particularly when lesions are located in anatomically difficult to access areas of the oral cavity, were major contributing factors [18]. In the present case, both initial symptom minimization and the patient’s refusal of a recommended biopsy, due to low cancer awareness, significantly contributed to the delay. Additionally, system-related issues such as poor interprofessional communication and lack of trust in the primary provider, as evidenced by the patient independently consulting another physician without intervention, further compounded the delay.
The five-year survival rate for oral cancer ranges between 55-68% [10,11]. Prognosis is strongly influenced by the tumor’s stage at the time of diagnosis, as defined by the TNM classification (AJCC 8th edition) [25]. In the presented case, the tumor was diagnosed at clinical stage T4N0M0, indicating local tissue invasion without nodal or distant metastases. According to data by Warnakulasuriya et al., the five-year survival rate for patients diagnosed at stage I is approximately 80%, while in advanced stages (III and IV), it drops to around 20% [8].
Delayed diagnosis not only significantly worsens the prognosis but also necessitates more extensive treatment, which can lead to numerous complications, functional impairments, and a substantial decline in quality of life [26]. In the described case, the patient underwent an extensive surgical procedure, followed by radiochemotherapy. Despite adhering to the principle of minimal invasiveness whenever possible, the advanced stage of the disease necessitated a wide range of therapeutic interventions. As a result, the patient required a prolonged recovery period and was at risk of developing functional complications such as speech disorders, dysphagia, and chronic pain - all typical in cases where oncological treatment begins at a later stage [27].
Additionally, late treatment-related complications, including weakened immunity and cachexia, may have contributed to the development of pneumonia, which ultimately led to the patient's death.
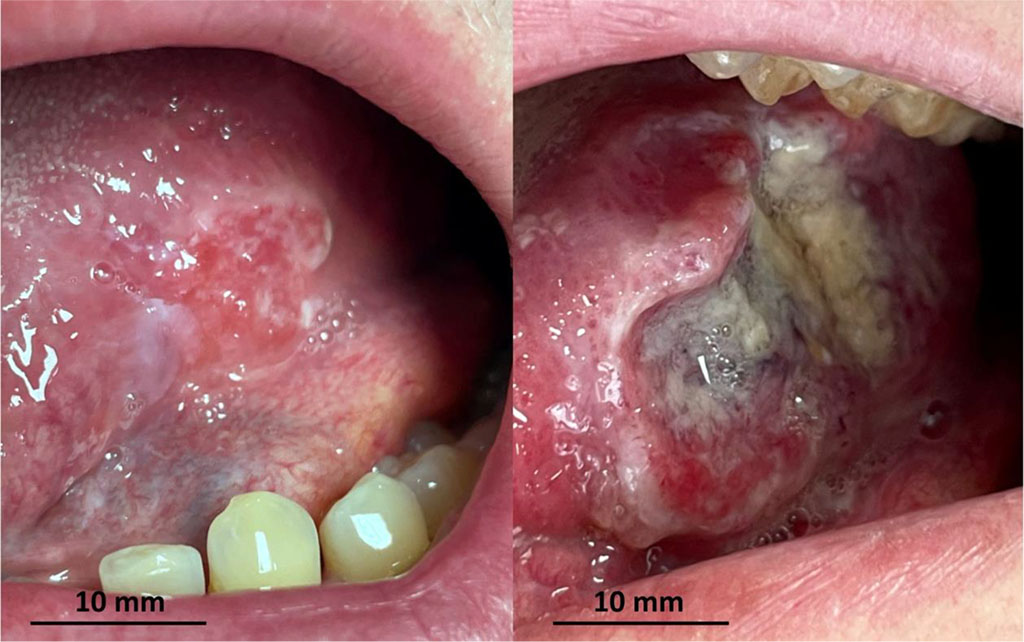
Fig. 2 2-month rapid progression of oral squamous cell carcinoma.
This case demonstrates that oral squamous cell carcinoma can progress rapidly even in patients without traditional risk factors such as tobacco use, alcohol consumption, or comorbidities. Delayed biopsy and missed opportunities for early intervention contributed to tumor progression and ultimately to a fatal outcome, despite histologically confirmed remission.
The case highlights several critical clinical lessons. First, persistent or atypical oral lesions require biopsy without delay, regardless of patient age or presumed risk status. Second, when consent is initially withheld, clinicians must clearly communicate the potential consequences and ensure short-interval follow-up. Third, conventional oral examination must be supplemented by decisive diagnostic action when malignancy cannot be excluded.
Interdisciplinary cooperation should not be limited to advanced disease management but must also be integrated into the early diagnostic process. Referral protocols, especially between dentists and oncologists, should be formalized to prevent loss of time during uncertain presentations.
Education efforts should address the rising incidence of oral cancer in younger and low-risk populations. Diagnostic vigilance must be maintained even in patients who do not fit the classical epidemiological profile.
Clinical protocols should be revised to include mandatory reassessment timelines for unresolved oral lesions and predefined escalation strategies when biopsy is postponed. Avoiding preventable delays can directly impact prognosis and treatment burden.
An informed consent for publication was obtained from the patient.
Conceptualization: N.S., B.L.; Photography and image preparation: N.S., B.L., Z.S., J.M.; Methodology: N.S., B.L., A.N.; Investigation: N.S., B.L., Z.S., J.M., W.T., P.S.; Formal analysis: A.N., M.L.; Writing – original draft: B.L., M.L. A.N.; J.M., Z.S., W.T., P.S.; Writing – review & editing: N.S., R.W., D.S.; Supervision: D.S., R.W.
All authors have read and agreed with the final version of the manuscript.
Artificial intelligence tools (e.g., ChatGPT, OpenAI) were used to assist in language editing, formatting suggestions, and structuring of the manuscript. The final content was critically reviewed and approved by the authors.
The study did not receive special funding.
The authors declare no conflicts of interest.