- Home
- About the Journal
- Peer Review
- Editorial Board
- For Authors
- Reviewer Recognition
- Archive
- Contact
- Impressum
- EWG e.V.
The article describes a clinical case of a rare zoonotic hair disease characteristic of countries with a tropical climate. Close contact between a sick person and a healthy person turned out to be the cause of a sporadic case of black piedra in Russia. The features of the epidemiology and clinical picture of this disease, methods of laboratory diagnosis and treatment are presented.
KEYWORDS: black piedra, sporadic case, epidemiology, clinical manifestations, diagnostics, treatment methods
Black piedra (Syn.: knotted trichosporia, tropical trichosporosis, knotted trichomycosis) is a rare anthroponotic hair disease manifested by the formation of hard, stony density of black nodules on them. The causative agent of the black piedra is the fungus Piedraria hortai. The infection was first described by Desenne in 1878 [12, 14].
The disease occurs in countries with hot, humid climates: in South America, India, Southeast Asia and Africa. In Europe, it is diagnosed quite rarely, mainly in immigrants. In Russia piedra occurs sporadically, mainly from Central Asia [9]. The disease is not contagious, but cases of simultaneous infection of several members of the same family have been described. Women aged 25 to 40 are more likely to get sick; this pathology is extremely rare in men and children. The life cycle of the black piedra takes place entirely in nodules on the surface of the hair [1, 14].
The mechanism of transmission of the disease is intra-household and close-contact. The spread of the disease occurs through combs, by wearing tight hats, bandages, and with close household contacts. The source of the disease is a sick person. Disruption of the integrity of the cuticle layer, the use of water from non-flowing reservoirs for washing the head, decoction of flaxseed, sour milk, as well as constant lubrication of the hair with vegetable oil, contribute to infection with piedra [12, 15].
The occurrence and spread of the disease are promoted by high temperature and a humid environment, as well as non-compliance with the rules of hygienic hair care. The pathogenicity factors of the fungal infection have not been sufficiently studied due to the rare occurrence of the disease. Many authors consider the black piedra not as an infection, but as epiphyte, that is, the existence of an organism on the surface of the host body, without penetration into its tissues [6, 12].
P. hortae forms dense black nodules on long hair of the head, usually in the distal third, and extremely rarely affects the hair of the beard and mustache. The nodules are mosaically arranged, tightly glued spores of the fungus, which can merge, forming a kind of hair case, up to 1 cm in length [9, 12]. Small, black, fusiform nodules 1–2 mm in diameter are usually visually visible on light hair. On dark hair, they can only be determined by palpation when conducting the affected hair between the fingers. Combing the hair affected by the piedra may be accompanied by a peculiar metallic sound. On long hair, the knots can interlock with each other and form a so-called “Columbian tangle”. Patients with black piedra do not experience subjective sensations, there are no specific rashes when examining the scalp. It is known that in the absence of piedra treatment, patients with concomitant diseases (diabetes, immunodeficiency, malignant tumors) may develop alopecia [7, 13].
In differential terms, trichoscopy is an indispensable diagnostic method. The manifestations of black piedra on the hair should be distinguished from pediculosis, but the absence of itching, the causative agent of the disease on the scalp and nits on the rod is a distinctive feature. However, white piedra is characterized by lighter and softer nodules observed during examination and dermatoscopy. The disease also needs to be distinguished from moniletrix, a genetic disease that leads to brittle hair and the appearance of thickenings resembling beads on it. And from knotty trichorexis, an acquired disease characterized by brittle hair and microscopic branched nodules throughout the hair shaft [2, 5, 11, 13].
The diagnosis of black piedra is made on the basis of a characteristic clinical picture confirmed by various diagnostic methods. The basis of the diagnosis is a microscopic examination of the pathological sample treated with a 10% KOH solution, which shows branched hyphae (from 4 to 8 microns) glued together with a cement-like substance. When sowing on a medium with dextrose Saburo agar (SDA), greenish-black colonies with a raised and medullary center grow. The study of rods using trichoscopy is also a highly informative method of diagnosing hair diseases [8, 13].
Methods of treatment described in the literature are diverse. Traditionally, hair shaving has been used as the simplest method of treatment, but this is unacceptable for women from an aesthetic point of view. Previously, hair was treated with a 10% hot solution of sulema or sulema vinegar, followed by combing out the nodules with a frequent comb. Currently, it is proposed to treat the hair web with various forms of antifungal agents. There are reports of the effectiveness of oral terbinafine 250 mg/day for 6 weeks. With timely treatment the prognosis is good, otherwise the disease may proceed chronically [3, 4, 10].
The purpose of this study was to demonstrate a sporadic case of black piedra in a young woman living in Russia.
Patient O., 35 years old, a teacher, works with students from India and Sri Lanka. In autumn, foreign students returned from the summer vacation. At the first lesson, students offered to take a memorable photo, which implied physical contact and, apparently, caused the infection.
After 2 months, the woman began to worry about the appearance of many dark nodules along the entire length of the hair. While collecting anamnesis, it became known that she had a habit of coming to work with wet hair, as she exercises every morning and often does not have time to dry her hair. During a visual examination, it was determined that the patient had thick, light hair, a lot of her hair had small dark-colored nodules, annularly covering the hair shaft and not removable when attempting mechanical removal (Fig.1).

Fig. 1 Hair of patient O. suffering from black piedra
During dermatoscopy of the affected hair rods, it became obvious that dark nodules in the form of oblong cases were visible (Fig. 2).
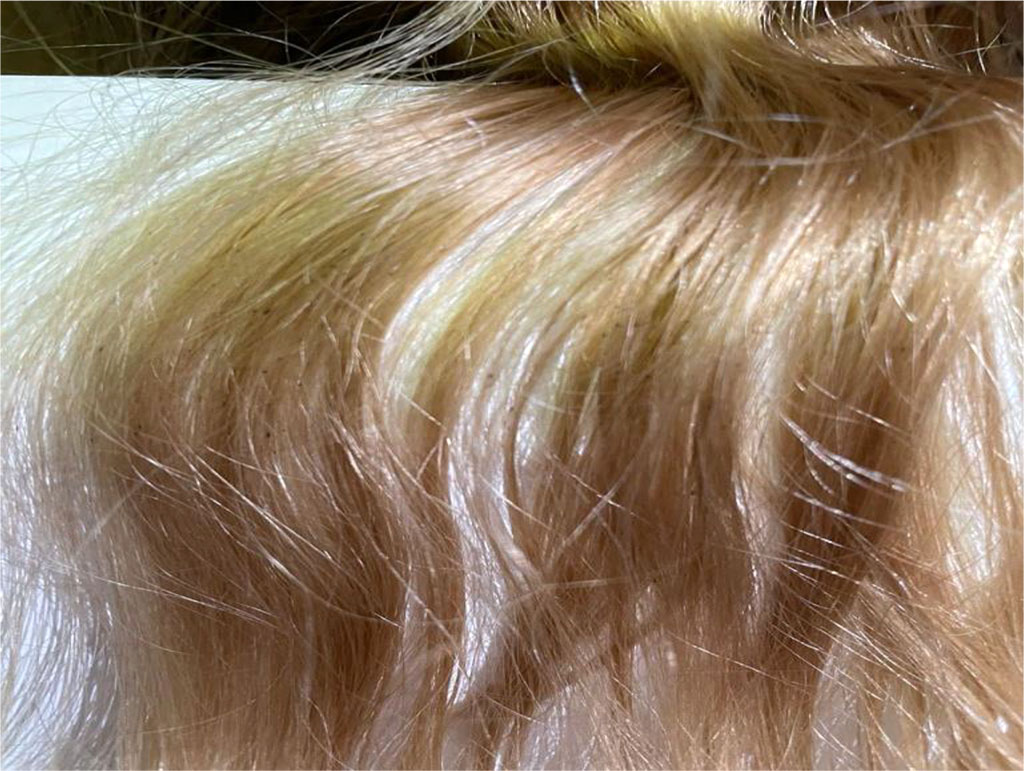
Fig. 2 Dermatoscopy of hair affected by black piedra (× 20)
The digital dermatoscope FotoFinder ATBM body studio was used for the examination, which allowed taking micrographs with a twenty-fold magnification. By direct microscopy with an increase of 400 times, after treating the hair with KOH solution, filamentous hyphae in the form of chains resembling arthrospores were found as well (Fig. 3). Sowing on Saburo medium did not give growth of the fungus.
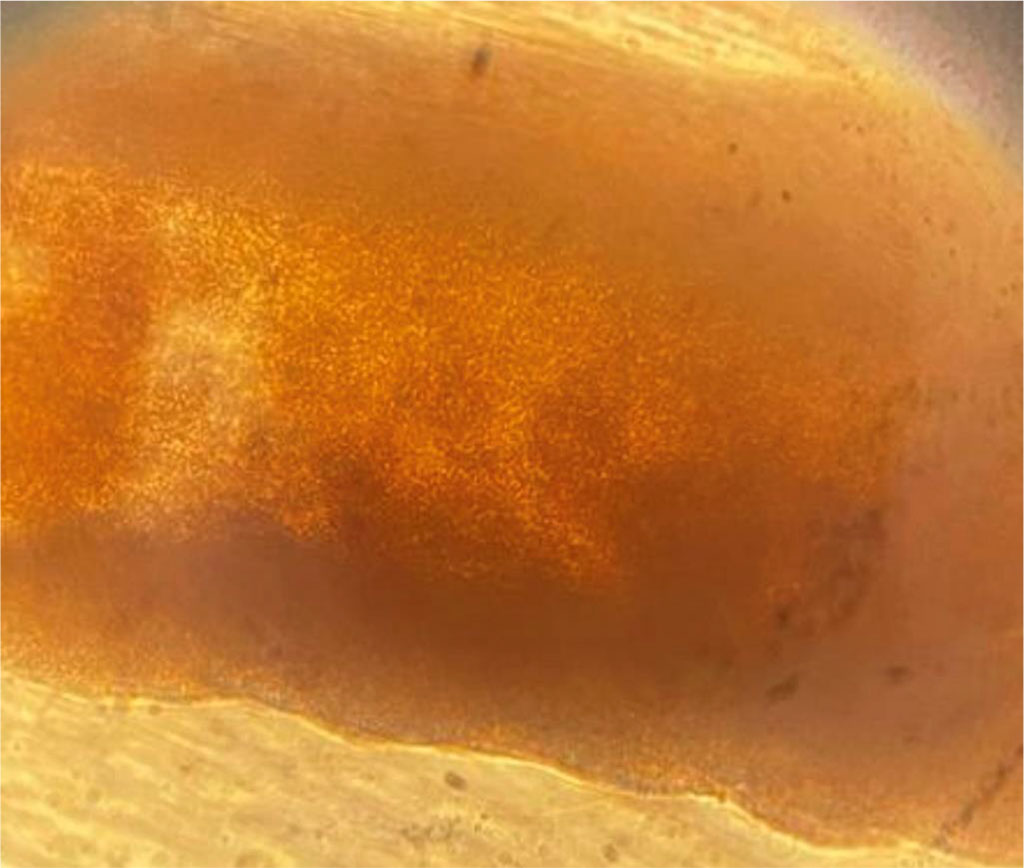
Fig. 3 Direct microscopy of hair affected by black piedra (× 400)
For 14 days, the external treatment was carried out: shampoo containing 2% ketoconazole, three times a week, with exposure, spray containing terbinafine, twice a day. Also, the heat treatment of the hair rods with a hot iron was carried out, which turned out to be very effective, since during this procedure, most of the dense rocky nodules independently broke off from the hair. Combing of the remaining elements with a frequent comb and disinfection of combs and bed linen were carried out daily.
This clinical case is of particular interest due to the rare occurrence of black piedra in Russia. Timely diagnosis of the disease, dermatoscopy data, and properly selected treatment led to a complete clinical recovery, preserving the patient's hair.