Erfolgreich durch internationale Zusammenarbeit
OPHTHALMOLOGY
Cite as: Archiv EuroMedica. 2024. 13; 1: e1. DOI 10.35630/2024/14/1.111
Received 10 February 2024;
Accepted
25 February 2024;
Published 26 February 2024
HEBREW TRANSLATION AND VALIDATION OF THE CATQUEST- 9SF QUESTIONNAIRE
Adi Porat Rein 1 
 , Matan Rosen2,
, Matan Rosen2,
Mats Lundström3  , Mor M. Dickman 4
, Mor M. Dickman 4  ,
,
Yaron Finkelman5, David Zadok1  ,
,
Adi Abulafia1 
1Department of Ophthalmology, Shaare
Zedek Medical Center, affiliated with the Hebrew University –
Hadassah School of Medicine, Jerusalem, Israel
2 Hebrew
University – Hadassah School of Medicine, Jerusalem,
Israel
3Department of Clinical Sciences/Ophthalmology,
Faculty of Medicine, Lund University, Lund, Sweden
4University
Eye Clinic, Maastricht University Medical Center, Maastricht, The
Netherlands
5 Eye CU clinic, Private clinic, Tel Aviv,
Israel
ABSTRACT
Aims: The purpose of this study is to translate and validate a Hebrew version of the Catquest-9SF questionnaire, an efficient patient-reported outcome measure (PROM), for the assessment of cataract surgery outcome
Methods: This is a prospective questionnaire validation study. The Catquest-9SFquestionnaire was translated from English to Hebrew following a standard procedure. The study population included candidates for cataract extraction surgery in both eyes. They were 21 years of age or older, Hebrew-speaking, and had Internet access. They completed the questionnaire in 2 stages, once before the surgery on the first eye and again 4-6 weeks following the surgery on the second eye. A Rasch analysis was performed to validate the Hebrew version of the questionnaire, and a sensitivity analysis was performed for the patients who completed both the preoperative and postoperative questionnaire.
Results: Of the 133 patients included in the study, 125 completed the first questionnaire, and 24 also completed the second questionnaire by the time of study closure. The Hebrew translation of Catquest-9SF demonstrated 1-dimensionality, ordered response categories and good person separation. The sensitivity analysis on the 24 paired Catquest-9SF questionnaires showed good effect size (1.85).
Conclusions: The Hebrew versions of the Catquest-9SF questionnaire is valid and reliable with psychometric properties of good quality and good effect size. It is applicable to Hebrew-speaking cataract patients for clinical assessment and research purposes.
Keywords: cataract surgery, patient-reported outcome, questionnaire, Hebrew translation, validation, Catquest-9SF.
INTRODUCTION
Cataract is a major cause of blindness worldwide, [1] and the outcome of visual acuity following cataract extraction surgery has become an increasingly important issue for patients [2] Various steps in current surgical approaches are instrumental in achieving the best postoperative visual outcome [3] Several questionnaires have been developed in order to monitor the patients' subjective assessment of their vision in order to determine whether and to what extent their expectations of improving their postoperative quality of life have been met. [4]
The Catquest questionnaire was originally developed in the Swedish language in 1995 [5] and the Catquest-9SF questionnaire is a shorter version which was developed by Lundstrom and Pesudovs in 2009 [6]. The Catquest-9SF questionnaire is designed to measure limitations in the individual's activities of daily living (ADL) due to the presence of cataracts.[6]
The Catquest-9SF questionnaires were developed with the use of a modern test theory (Rasch analysis) [6]. Patient-reported outcome measures (PROMs) assessed the patients' perceptions of their vision, and thereby drive improvement in healthcare. The questionnaire is an efficient PROM tool for the assessment of cataract surgery outcome. [7] It has been validated, and is used by the European Society of Cataract & Refractive Surgeons (ESCRS) in several languages, making them applicable for use in multinational studies and research.
In order to accurately reflect the subjective responses to the questionnaire’ items, it is important that it would be written in the patient’s commonly used language. Furthermore, different cultures and populations comprehend and relate to the questions according to their cultural, educational, demographic characteristics, and more.[8] It is therefore essential for the questionnaire to be translated and validated for adaptation to each population.[9]
To the best of our knowledge, there is no standardized vision PROM in clinical practice in the Hebrew language. We contend that the translation and validation of the questionnaire in Hebrew will support self-auditing as well as expand the Israeli contribution to national and international clinical studies on the subjective outcomes of cataract surgery. Toward these ends, we translated and validated the Catquest-9SFquestionnaire from English to Hebrew.
METHODS
Translation
This study conformed to the Declaration of Helsinki and was approved by the Shaare Zedek Medical Center Institutional Review Board.
Two translators who are fluent in both English and Hebrew translated the Catquest-9SF questionnaire from English to Hebrew by the protocol "forward translation”[10] . This preliminary version was translated from Hebrew to English by a process known as "backward translation"[10] by 2 other translators who are also fluent in both languages. The translators and the study investigators then reviewed the findings, resulting in a single unified document in the Hebrew language. This draft was administered to 5 patients who had undergone cataract surgery and were attending the Shaare Zedek Medical Center's outpatient eye clinic. They filled in a brief form to provide feedback on the content and ease of understanding the Hebrew questionnaires. Adjustments were made according to their comments, and the translated version of the questionnaire was finalized. The original Catquest-9SF questionnaire is publicly available and a license is not needed for use, through the standard sets for cataract in the International Consortium for Health Outcomes Measurement (ICHOM). In addition, a permission obtained from the questionnaire author (M.L).
Data Collection
This was a prospective questionnaire study. The participants were recruited from the Ophthalmology Department at Shaare Zedek Medical Center, Jerusalem, Israel. They all voluntarily entered the study and signed an informed consent form. The inclusion criteria were a diagnosis of cataract in both eyes, a minimum age of 21 years, fluency in Hebrew and access to the Internet. Patients with severe cognitive impairment, pregnancy (current or planned) or lactating, as well as those who were unable to complete follow-up visits were excluded. The data were collected from 133 patients (55 males, 78 females, average age 71.9 years [range 40-94]) from November 2021 to August 2022. The first questionnaire was completed in either an electronic or paper-based form during the preoperative visit. The second questionnaire were completed 4-6 weeks after the second eye surgery, either at the clinic by means of a paper-based form or at home by a digital form returned by e-mail. The authors had access to information that could identify individual participants during the data collection only.
Statistical Analysis
The Hebrew questionnaire was validated with the Rasch analysis (version 5.3.2 of Winsteps Chicago, IL, USA), a statistical model commonly used to validate PROM questionnaires.[11]
The Catquest-9SF questionnaire includes 9 items: 7 questions pertaining to ADL and one question pertaining to general sense of difficulty. The 5 choices of responses were "very great difficulty", "great difficulty", "some difficulty", "no difficulty" and "cannot decide". The 9th question pertained to satisfaction in postoperative vision, and the choices of responses were "very dissatisfied", "rather dissatisfied", "fairly satisfied", "very satisfied", and "cannot decide".
The Rasch analysis is a statistical model used to differentiate between items according to their level of difficulty, thereby enabling the evaluation of the participants and their separation into different profiles or groups according to their responses. The effect size was based upon the results of the Rasch analysis according to the following formula: the postoperative mean Rasch score minus the preoperative mean Rasch score divided by the standard deviation (SD) of the preoperative score.
RESULTS
One-hundred and thirty-three consecutive patients were included in the study between November 2021 to August 2022. Of them, 125 (93.98%) completed the questionnaire. Eight patients (6.02%) were excluded, 4 due to technical issues and 4 due to missing answers. Forty-one (30.83%) patients underwent a second-eye surgery, and 24 of them completed the questionnaire for the second time by the time of study closure. The participants' demographic and refraction data are summarized in [Table 1].
Table 1. Patient demographics and best corrected visual acuity before and after cataract surgery in both eyes
| Filled in both the preoperative and postoperative questionnaires | Filled in only the preoperative questionnaire | |
| 24 | 133 | Number of patients |
| 68.6 ± 12.1 (40-88) | 71.9 ± 10.2 (40-94) | Mean age ± SD, yr (range) |
| 13 (54.16%) | 78 (58.65%) | Female sex |
| 0.10 ± 0.16 | 0.33 ± 0.22 | BCVA right eye (logMAR) ± SD |
| 0.09 ± 0.15 | 0.32 ± 0.23 | BCVA left eye (logMAR) ± SD |
BCVA = best corrected visual acuity, SD = standard deviation
Catquest 9SF Validation
Rasch analysis-determined good precision was calculated by a person separation of 2.20 and a person reliability of 0.83. In addition, the infit mean square varied between 1.46–0.68 and the outfit mean square varied between 1.24–0.63. There was no significant misfit, although item 4 showed a slight misfit as an outlier and item 9 showed a slight misfit because of redundancy. The category probability curves indicated that respondents could separate the responses based upon the response options [Figure 1a]. A person-item map [Figure 1b] determined how well the items had been targeted to the abilities of the survey participants. Based upon the difference in mean values (logit), it was concluded that the participants were more able than the items were difficult, with a difference of 0.93 logits.
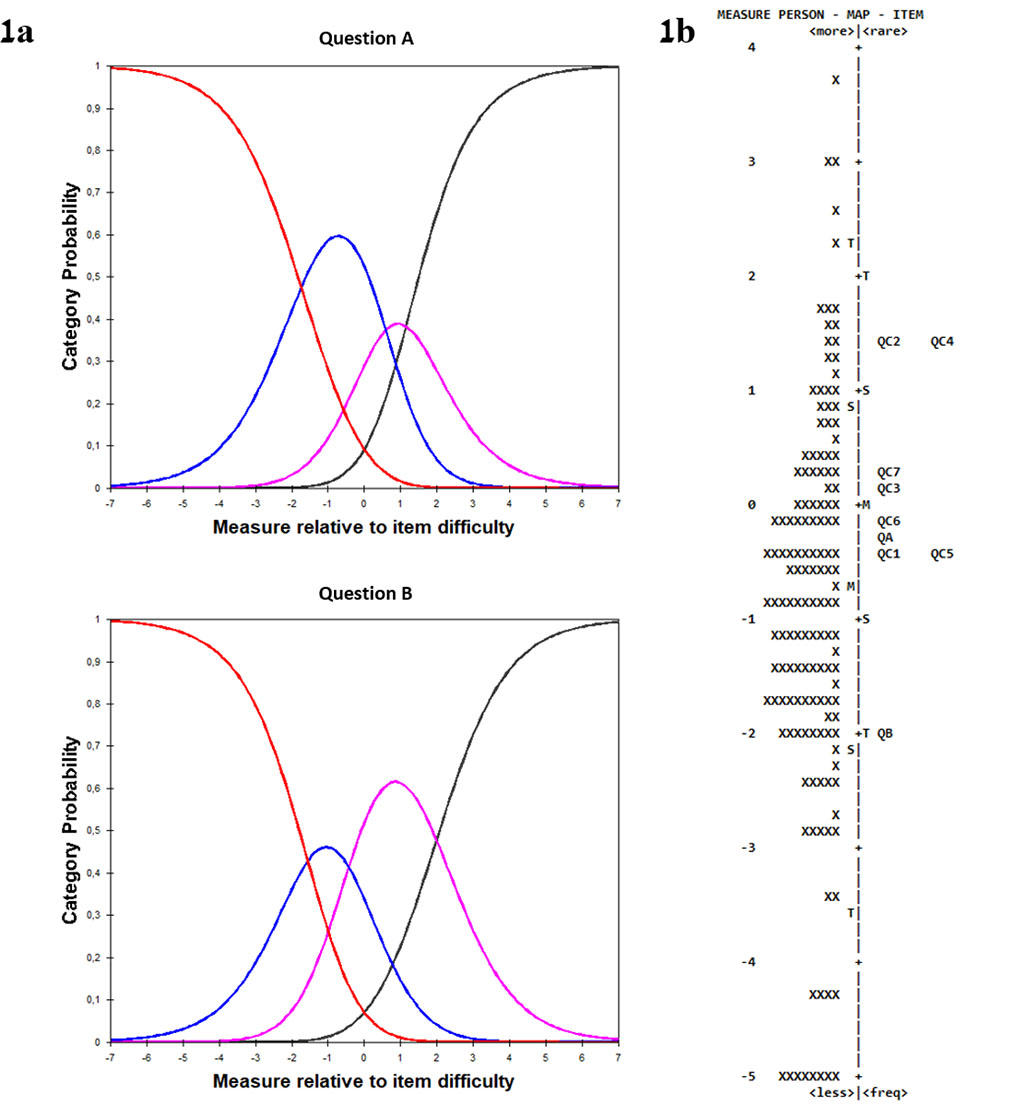
Fig. 1. Catquest-9SF Rasch analysis
1a. Questions A
and B probability curves. 1b. Person-item map. The items are on the
right and the patients are on the left.
Sensitivity analysis
The effect size was calculated as postoperative mean Rasch score (-0.91) minus the preoperative mean Rasch score (0.92) divided by the SD of the preoperative score (0.99). The effect size for Catquest-9SF was 1.85 based upon the 24 preoperative and 24 postoperative questionnaires completed by the same 24 individuals.
DISCUSSION
We translated the Catquest-9SF questionnaire from English to Hebrew following a standard procedure and verified its reliability and validity by means of Rasch analysis. To the best of our knowledge, there is no valid Hebrew questionnaire designed to assess cataract treatment or subjective quality of vision in patients with cataract and following cataract surgery. The Catquest-9SF questionnaire showed good fit with good effect size.
The Catquest-9SF questionnaire had been translated and validated in many languages.[12–16] When designing the Catquest questionnaire, Lundstrom et al. observed that the outcomes of cataract surgery cannot be based solely upon visual acuity, mainly because the patient's assessments, including those of visual perception, ADL and disabilities due to vision are crucial.[7]
There are several aspects that bestow great importance to the validation of the Hebrew Catquest-9SF questionnaire. First, the translation ensures that the questionnaire will be understood by Hebrew speakers both linguistically and culturally. Second, it is beneficial in providing the surgeon with direct knowledge of various aspects of the patient's quality of life and enabling an open dialogue regarding the patient's expectations for the purpose of planning the surgery. Third, it provides validated tools for auditing and research purposes. Importantly, Israel, like many other countries, will be able to supplement the derived data when conducting multi-institutional studies on cataract surgery involving national and international medical centers.
There are several limitations to our study. By responding to a written questionnaire in the clinic, the patient may be influenced by the presence of the surgeon and the desire to please him/her when answering the questionnaire, thus creating a bias. Therefore, the post-operative PROMs in our study were administered digitally or by an optometrist. In addition, patients may miss a question in the questionnaires due to lack of attention, thereby being excluded from the study. It is also important to note that any questionnaire study includes an element of intermediate situations that may not entirely fit the pattern that is queried, and the patient may be obliged to compromise his/her answer to fit one of the provided answers. Since the sensitivity analysis of the questionnaire was conducted on a small number of postoperative questionnaires (n = 24), a repeated sensitivity analysis with a greater number of questionnaires will be required to validate our results.
CONCLUSION
The Catquest-9SF questionnaire was translated from English into Hebrew and successfully validated. The Rasch analysis demonstrated that it can be used by a Hebrew-speaking population with high reliability and validity. The questionnaire can provide expanded evidence on Israeli patients for use in national studies in the cataract field, as well as in international collaborations in future ophthalmology research.
ACKNOWLEDGEMENTS
This study was performed in partial fulfillment of the requirements for the degree of medical doctor, Faculty of Medicine, Hadassah Medical School of the Hebrew University, Jerusalem. We acknowledge Yehudit Bardugo and her staff for their contribution to the completion of the patients’ questionnaires process.
AUTHOR CONTRIBUTIONS
All co-authors meet the requirements for authorship and equal contribution. They have all reviewed and approved the contents of the manuscript.
STATEMENTS AND DECLARATIONS
The authors declare that no funds, grants, or other support were received during the preparation of this manuscript. The authors have no conflicts of interest to declare that are relevant to the content of this article.
REFERENCES
- Olson RJ, Braga-Mele R, Chen SH, Miller KM, Pineda R, Tweeten JP, et al. Cataract in the Adult Eye Preferred Practice Pattern®. Ophthalmology. 2017 Feb 1;124(2):P1–119. DOI: 10.1016/j.ophtha.2016.09.027
- Aristodemou P, Sparrow JM, Kaye S. Evaluating Refractive Outcomes after Cataract Surgery. Ophthalmology. 2019 Jan 1;126(1):13–8. DOI: 10.1016/j.ophtha.2018.07.009
- Kane JX, Van Heerden A, Atik A, Petsoglou C. Accuracy of 3 new methods for intraocular lens power selection. J Cataract Refract Surg. 2017 Mar 1;43(3):333–9. DOI: 10.1016/j.jcrs.2016.12.021
- McAlinden C, Gothwal VK, Khadka J, Wright TA, Lamoureux EL, Pesudovs K. A Head-to-Head Comparison of 16 Cataract Surgery Outcome Questionnaires. Ophthalmology. 2011 Dec 1;118(12):2374–81. DOI: 10.1016/j.ophtha.2011.06.008
- Lundström M, Brege KG, Florén I, Stenevi U, Thorburn W. Impaired visual function after cataract surgery assessed using the Catquest questionnaire. J Cataract Refract Surg. 2000 Jan 1;26(1):101–8. DOI: 10.1016/s0886-3350(99)00324-7
- Lundström M, Pesudovs K. Catquest-9SF patient outcomes questionnaire. Nine-item short-form Rasch-scaled revision of the Catquest questionnaire. J Cataract Refract Surg. 2009 Mar;35(3):504–13. DOI: 10.1016/j.jcrs.2008.11.038
- Lundstrom M, Roos P, Jensen S, Fregell G. Catquest questionnaire for use in cataract surgery care: Description, validity, and reliability. J Cataract Refract Surg. 1997;23(8):1226–36. DOI: 10.1016/s0886-3350(97)80321-5
- Wild D, Grove A, Martin M, Eremenco S, McElroy S, Verjee-Lorenz A, et al. Principles of good practice for the translation and cultural adaptation process for patient-reported outcomes (PRO) measures: Report of the ISPOR Task Force for Translation and Cultural Adaptation. Value in Health. 2005;8(2):94–104. DOI: 10.1111/j.1524-4733.2005.04054.x
- Kabanovski A, Hatch W, Chaudhary V, El-Defrawy S, Reid R, Ahmed IIK, et al. Validation and application of Catquest-9SF in various populations: A systematic review. Surv Ophthalmol. 2020 May 1;65(3):348–60. DOI: 10.1016/j.survophthal.2019.12.002
- Wild D, Grove A, Martin M, Eremenco S, McElroy S, Verjee-Lorenz A, et al. Principles of Good Practice for the Translation and Cultural Adaptation Process for Patient-Reported Outcomes (PRO) Measures: Report of the ISPOR Task Force for Translation and Cultural Adaptation. Value in Health. 2005 Mar 1;8(2):94–104. DOI: 10.1111/j.1524-4733.2005.04054.x
- Nguyen TH, Han HR, Kim MT, Chan KS. An Introduction to Item Response Theory for Patient-Reported Outcome Measurement. The Patient - Patient-Centered Outcomes Research 2014 7:1. 2014 Jan 9;7(1):23–35. DOI: 10.1007/s40271-013-0041-0
- Lundström M, Llovet F, Llovet A, Martinez del Pozo M, Mompean B, González JV, et al. Validation of the Spanish Catquest-9SF in patients with a monofocal or trifocal intraocular lens. J Cataract Refract Surg. 2016 Dec 1;42(12):1791–6. DOI: 10.1016/j.jcrs.2016.10.011
- Visser MS, Dieleman M, Klijn S, Timman R, Lundström M, Busschbach JJV, et al. Validation, test–retest reliability and norm scores for the Dutch Catquest-9SF. Acta Ophthalmol. 2017 May 1;95(3):312–9. DOI: 10.1111/aos.13287
- Adnan TH, Mohamed Apandi M, Kamaruddin H, Salowi MA, Law KB, Haniff J, et al. Catquest-9SF questionnaire: validation of Malay and Chinese-language versions using Rasch analysis. Health Qual Life Outcomes. 2018 Jan 5;16(1):5. DOI: 10.1186/s12955-017-0833-3
- Skiadaresi E, Ravalico G, Polizzi S, Lundström M, González-Andrades M, McAlinden C. The Italian Catquest-9SF cataract questionnaire: translation, validation and application. Eye and Vision. 2016 Dec 1;3(1):1–8. doi: 10.1186/s40662-016-0043-9
- Katz G, Rouquette A, Lignereux F, Mourgues T, Weber M, Lundström M. Validity of the French version of Catquest-9SF and use of an electronic notepad for entering patient-reported outcome measures. Eye and Vision. 2021 Dec 1;8(1):1–9. doi: 10.1186/s40662-021-00233-7